Introduction
At Dr. Lenia’s Dental Surgery in Paphos, Cyprus, we firmly believe that oral health is a direct reflection of the body’s overall health. For this reason, every time a patient undergoes a complex dental procedure – such as a simple extraction or oral surgery – our team is committed to carefully considering the entire clinical picture, including the use of long-term medications. This holistic approach is the key to ensuring treatments are not only effective but, above all, safe.
Today, we want to address a vitally important topic that concerns a significant number of patients, particularly those who have received an osteoporosis diagnosis and are following specific pharmacological therapies. If you are taking medication for osteoporosis and need to visit the dentist, it is essential that you read the following carefully. We will explain why these treatments, although crucial for preventing fractures and strengthening your bones, can interact with jawbone healing and, consequently, require a high level of specialized attention and preparation on our part. Let’s delve immediately into what these drugs are and why knowledge of them is an essential element of your patient file.
Defining Osteoporosis: A Silent Disease
Before exploring the interaction between medications and oral health, it is essential that we understand exactly what osteoporosis is and why it is a condition that requires multidisciplinary attention.
What is Osteoporosis
Osteoporosis is defined as a systemic skeletal disease characterized by reduced bone mineral density and deterioration of the microarchitecture of bone tissue. In simple terms, the bone progressively becomes more porous and fragile. Imagine the internal structure of your bones as a sponge: in a healthy person, the sponge is dense and robust; in those suffering from osteoporosis, the “holes” widen, compromising the mechanical strength of the bone itself. This fragility has a direct and often dramatic consequence: it exponentially increases the risk of fractures, even following minimal trauma that would not normally cause damage. The most common fracture sites are the hip, spine, and wrist.
Who It Affects
We emphasize that, although osteoporosis can affect anyone, it is particularly prevalent in certain demographic groups. It is an extremely common public health problem, especially among post-menopausal women. This is due to the decline in estrogen, hormones that play a crucial role in maintaining bone density. However, older men and people with certain medical conditions or who take specific medications (such as corticosteroids) can also develop this disease. Recognizing this prevalence is fundamental for us at Dr. Lenia’s Dental Surgery in Paphos, as the average age and clinical profile of our patients require us to always consider the potential risk of osteoporosis and act accordingly, both in diagnosis and treatment planning.
Osteoporosis Medications: The "Cure" (and the Risk)
Osteoporosis treatment relies on the use of medications aimed at slowing down bone loss, thereby increasing mineral density and reducing the risk of fractures. It is important to know that most of these drugs work by modifying the natural process of bone remodeling—a continuous cycle of bone breakdown (resorption) and building (formation). When this delicate balance is altered, unexpected interactions can arise in areas with high bone turnover, such as our maxilla (upper jaw) and mandible (lower jaw).
The Most Relevant Classes of Drugs
The medications that cause the most concern for us dentists primarily fall into two categories:
Class of Medication | Common Examples (Active Ingredients) | Mechanism of Action |
|---|---|---|
Bisphosphonates (BP) | Alendronate (oral), Risedronate (oral), Zoledronate (intravenous) | They act by potently inhibiting osteoclasts (the cells responsible for bone breakdown). The bone, not being “demolished,” becomes denser. |
Denosumab | Prolia (administered via injection) | This is a monoclonal antibody. It blocks the RANKL protein, which is essential for the survival and activity of osteoclasts, achieving an effect similar to BPs, but with a different mechanism of action. |
While other treatments exist, such as hormonal therapies or anabolics (which stimulate bone formation), Bisphosphonates and Denosumab are the drugs that present the greatest impact on managing dental surgical risk.
What Are the General Side Effects
Like all potent medications, those for osteoporosis can also have systemic side effects. For example, oral Bisphosphonates can sometimes cause gastrointestinal disturbances, while injectable forms or drugs like Denosumab may be associated with muscle pain or injection site reactions.
However, it is crucial for us dentists and for you patients that the focus shifts to a specific and very rare side effect that has a direct and serious impact on oral health: Medication-Related Osteonecrosis of the Jaw (MRONJ). This risk, though low, is the main reason why it is vital to always communicate your pharmacological history to us.
The Crucial Side Effect: Osteonecrosis of the Jaw (MRONJ)
After understanding the action of osteoporosis medications and the dentist’s role regarding drugs like Bisphosphonates and Denosumab, we must address the side effect, albeit rare, that requires our utmost professional caution: Medication-Related Osteonecrosis of the Jaw (MRONJ).
What is MRONJ
MRONJ is a severe but infrequent condition where the jawbone, following trauma or spontaneously, undergoes necrosis—meaning it dies—becoming exposed in the mouth without managing to heal for a prolonged period (typically more than eight weeks). The causes of this vulnerability are found precisely in the action of anti-resorptive drugs. The bone, unable to renew itself due to the osteoclast blockade induced by the drugs, loses its ability to repair damage, leaving it vulnerable to infection and collapse.
Why are the Maxilla and Mandible at Risk
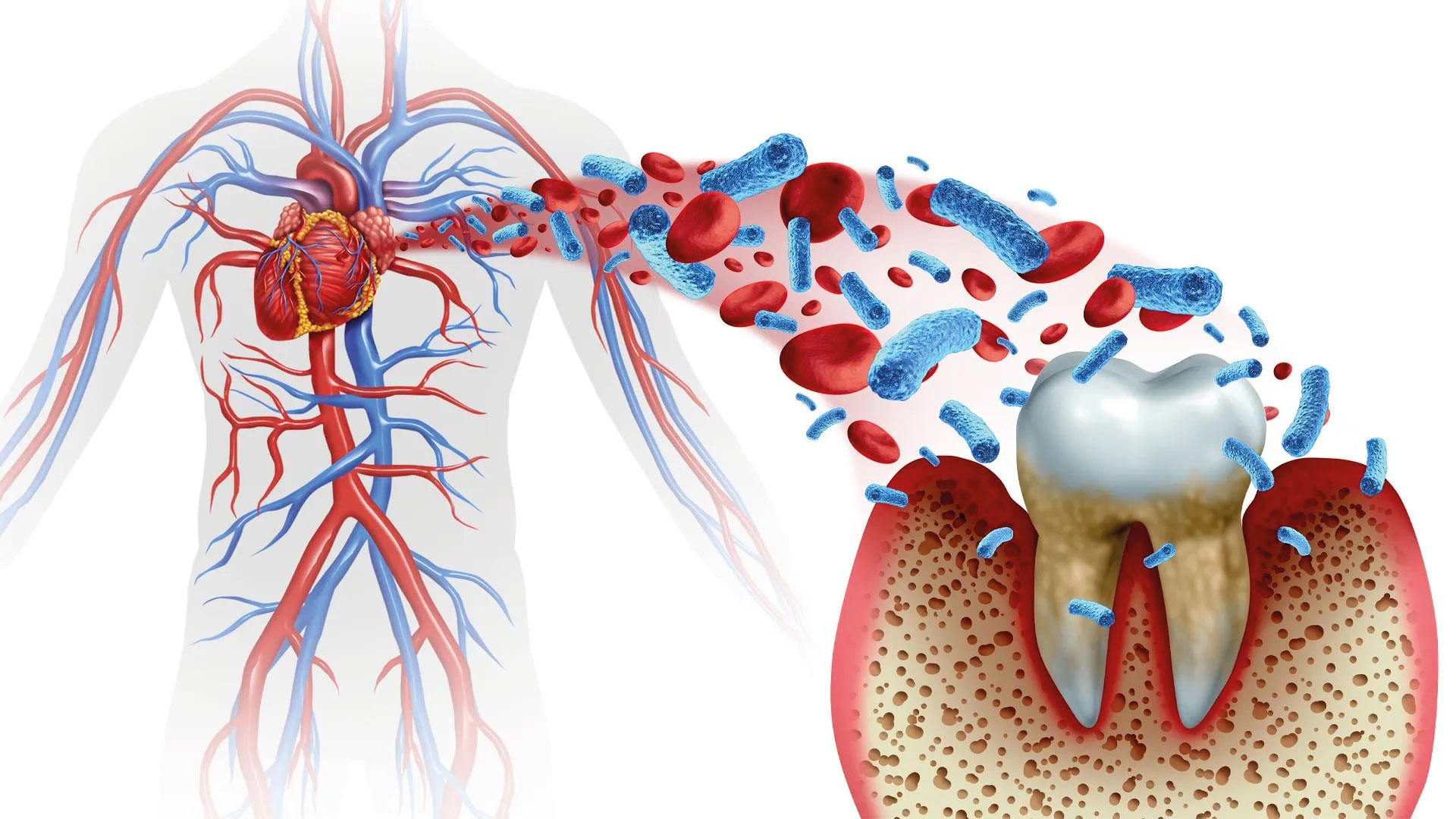
One might wonder why problems are concentrated in the mouth when the drugs were prescribed for long bones. The reason is structural: the maxilla and mandible, among all bones, have the highest turnover, meaning they renew themselves most rapidly and undergo significant daily mechanical stress (chewing). Furthermore, the oral environment is rich in bacteria, which can easily infiltrate compromised bone, turning minor trauma into a serious infection.
Extractions and Surgery: The Main Triggering Factors
MRONJ can occur spontaneously, but in most cases, it is triggered by events that cause trauma and require bone repair.
- Dental Extractions: These represent the most significant risk factor. An extraction creates a wound in the bone that heals quickly in a healthy patient. In a patient taking these osteoporosis medications, the bone’s healing capacity is inhibited, and the extraction site may never close properly, leading to bone exposure and infection.
- Other Surgical Interventions: Any procedure involving bone tissue, such as implant placement, periodontal surgery, or wisdom tooth removal, increases the risk.
- Advanced Periodontal Disease: Even a severe, chronic gum infection can expose the bone and trigger necrosis.
For this reason, it is fundamental that we dentists are aware of every therapy you are following, so that we can adopt stringent prevention protocols even before the intervention is necessary.
Why the Dentist Must Know (and What We Do for You)
Knowledge of your anti-osteoporosis therapy is not a detail, but a fundamental requirement to ensure your safety and the success of any invasive dental treatment. As we have seen, MRONJ prevention begins long before a tooth needs to be extracted.
Risk Assessment and Detailed Anamnesis
The first step we take at Dr. Lenia’s Dental Surgery is a detailed medical history (anamnesis). We don’t just ask if you are taking medication; we specifically ask how long you have been taking osteoporosis medications, how often (oral or intravenous/injection), and if you have ever received Denosumab (Prolia) injections. Based on this information, our team is able to classify your risk profile according to the latest international guidelines.
This evaluation is essential for deciding whether the required procedure can be performed routinely or if special precautions are needed.
Safe Treatment Protocols
If the risk is considered significant, especially before a dental extraction or surgical procedure, we adopt stringent safety protocols:
- Maximum Conservative Prevention: Our primary goal is always to avoid extraction, thereby eliminating surgical risk.
- Minimally Invasive Surgical Techniques: If extraction is unavoidable, Dr. Lenia and her staff perform the procedure using techniques that are as atraumatic and minimally invasive as possible to reduce bone damage to a minimum.
- Primary Suture: Often, to protect the exposed bone immediately after extraction, we completely close the wound with sutures so that the bone is never in contact with the oral environment and bacteria.
- Targeted Antibiotic Therapy: Preventive antibiotic therapy may be prescribed before and after the procedure to drastically reduce the risk of infection.
- Communication with the Treating Physician: In complex cases, we actively collaborate with your primary care physician to evaluate specific protocols, ensuring that every decision is multidisciplinary and safe.
The Cautionary Suspension Protocol (Drug Holiday)
In some cases (generally when oral Bisphosphonates have been taken for more than three years), the dentist may suggest that the patient ask their treating physician for a cautionary suspension (drug holiday) of the medication before the procedure.
Caution: This suspension must always be decided and managed exclusively by the prescribing doctor (endocrinologist or primary care physician), as suspension can increase the risk of fractures. For oral Bisphosphonates, the suspension typically lasts three months before and after the procedure; for drugs like Denosumab, suspension is often discouraged, and it is preferred to delay the dental appointment to utilize a safer “therapeutic window.”
Your cooperation in providing us with a complete clinical picture allows us to plan every step in a targeted and safe manner, transforming a potential risk into a successful clinical management.
Conclusion
Patient safety is the pillar upon which our clinical practice is founded. For this reason, transparent information and communication are the most effective weapons we can use against the potential risks arising from pharmacological interactions.
Our appeal is clear: If you are taking medication for osteoporosis, we ask that you provide this information to our team during the anamnesis stage. Not only do we ensure that our staff is fully updated on the latest clinical protocols to minimize the risk of MRONJ (Osteonecrosis), but we are also ready to work proactively and in synergy with your treating physician. Collaboration between specialists is essential for defining the safest and most personalized treatment plan for you.
Our goal, here at Dr. Lenia’s Dental Surgery in Paphos, Cyprus, is to ensure you receive excellent care in an environment that fully protects your overall health.
For an in-depth consultation and to discuss your specific situation with a prepared team, we invite you to contact our reception.
📞 For an appointment, call us at +357 26 946863.